
How COVID-19 has disproportionately affected US Latinos
How COVID-19 has disproportionately affected US Latinos
By July of 2020, months into the coronavirus pandemic, Latinos comprised a third of all COVID-19 cases in the United States.
While the virus infects bodies regardless of demographic or social status, various factors—from jobs to health care access—put certain groups at greater risk. These structural inequalities have played significant roles in disadvantaging the health of people of color for decades, whether "Asthma Alley" in the South Bronx or water quality issues in Flint, Michigan. But the pandemic has put a renewed spotlight on how such inequities disproportionately affect different groups of people.
Stacker analyzed data from the CDC, Census, and other surveys to explore how COVID-19 has disproportionately affected the American Latino community. Latinos represent a higher rate of essential workers and a lower rate of COVID-19 vaccinations. Of unvaccinated Latinos, a third report wanting the shot, compared to only 16% of unvaccinated whites, according to a Kaiser Family Foundation survey released in May 2021.
Keep reading for a look at how COVID-19 has disproportionately impacted Latinos, from health care access to housing conditions.

Hispanic and Latino people account for disproportionately high cases
Hispanic and Latino communities are overrepresented in COVID-19 case counts, representing just 18.45% of the population but 27.1% of all cases, according to the CDC. A number of overlapping economic, occupational, and cultural factors may contribute to this overrepresentation. Among these is a lack of access to quality health care, high-risk, non-remote jobs that increase potential exposure to the virus. Systemic inequalities that Hispanic and Latino populations face that lead to conditions like obesity and overcrowded housing can also increase the risk of exposure to COVID-19.

Case disparities are also prevalent at the state level
At the state level, these COVID-19 case disparities are also prevalent, particularly in states like California where Latinos make up a significant share of the population. To wit, California is 39.3% Latino but makes up 53.8% of COVID-19 cases. Stanford researchers posited that structural issues of inequality contribute to the high caseload in California, additionally concluding that racism itself may play a role in the high caseload.
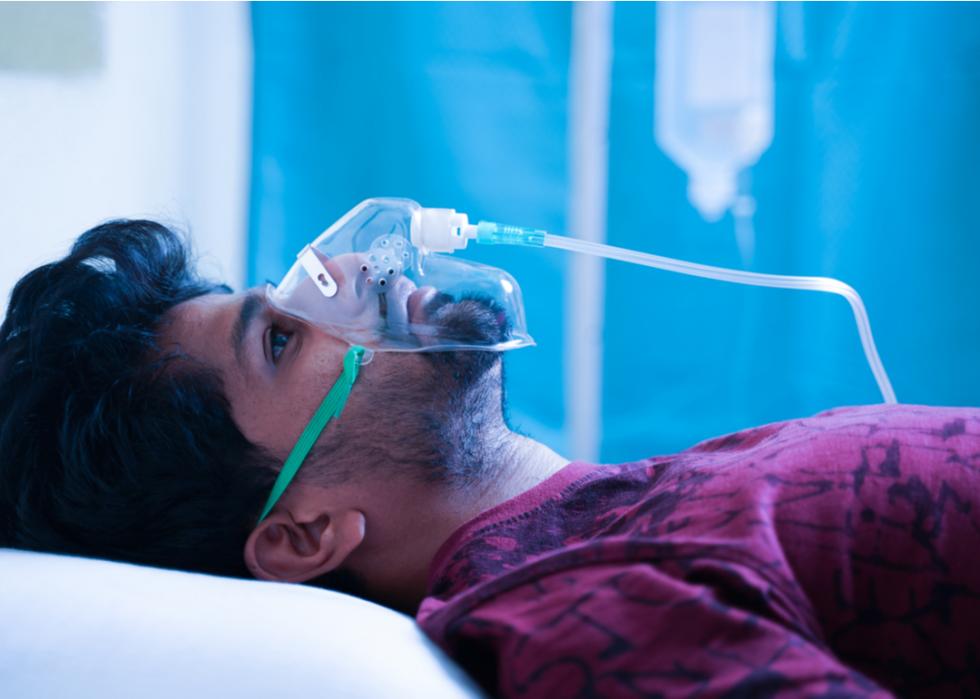
Hispanic and Latino people are more likely to be hospitalized
CDC data shows Hispanic and Latino people are 2.8 times more likely to be hospitalized for COVID-19 than non-Hispanic, white people. This may in part be due to factors that put Hispanic and Latino people at greater risk for severe disease, such as obesity. The CDC has reported that Latinos are the minority group with the second-highest rate of obesity in the country. Data from the CDC indicate a correlation between obesity and triple the risk of COVID-19 hospitalizations.

Hispanic and Latino people are more likely to die from COVID-19
Hispanic and Latino people are also 2.3 times more likely to die from COVID-19 compared to non-Hispanic, white people. The same factors that lead Hispanic and Latino populations to be hospitalized with COVID-19 also lead to a higher propensity toward death.
High blood pressure is one condition that can lead to an increased risk of severe COVID-19. Multiple studies have found that Hispanics have a higher rate of high blood pressure than the general population, and as such may be more susceptible to dying from COVID-19.

More Hispanic and Latino people experience food insecurity
Between April and May 2021, 15.4% of Hispanic/Latino people reported to the Census Bureau's monthly Household Pulse Survey that their households sometimes or often didn't have enough food to eat in the week prior, compared to 9.82% of the general population. This disparity has held true throughout the pandemic.
The most recently available data from a late August 2021 survey showed 13.4% of Hispanic/Latino respondents were experiencing food insufficiency compared to 8.56% overall. One reason for this disparity may be the types of work Hispanic and Latino populations are overrepresented in, such as in the hotel and leisure industry. These industries, which experienced a sharp reduction in demand during the pandemic, may have been quick to lay off workers—making it more difficult for people to buy food for themselves and their families.

Hispanic and Latino people suffered high rates of employment loss
At the start of the pandemic, 47% of people experienced a loss of employment income, according to the Household Pulse Survey. For Hispanic and Latino respondents, this jumped to 58%. Latinos are overrepresented in service industry jobs, such as working as Uber drivers. When the pandemic hit, many service-based professions were faced with a devastating lack of work as remote workers hunkered down at home, leading to employment loss for those who provide services to people outside the home.

Hispanic and Latino people had the least access to remote work
Hispanic and Latino people had the least access to remote work during the pandemic. In May 2020, 35.4% of the general population could work from home, compared to 23% of Hispanic/Latino people, according to data from the Bureau of Labor Statistics.
Jobs like food delivery, factory work, and food processing cannot be done while quarantining at home. As such, those working in such occupations were at increased risk for exposure to the virus. This increased exposure is particularly dangerous when considered with the factors that lead to COVID-19 being disproportionately dangerous for U.S. Latinos, as one of the most at-risk groups has some of the highest exposure rates.

Many Hispanic and Latino people struggled to pay rent
At the start of the pandemic, 17% of Hispanic/Latino Household Pulse respondents and 15.14% of all respondents couldn't pay their rent. The most recent survey shows 18.4% of Hispanic/Latino households in renter-occupied units were not caught up on rent, compared to 14.6% overall.
Due to the economic insecurity of service-based jobs that Latinos are overrepresented in, income loss has been prevalent among Latinos during the pandemic. This loss of income likely contributed to the inability to pay rent. Those with comorbidities like high blood pressure that put them at increased risk of severe COVID-19 may have been faced with the difficult decision between going out to look for service work and paying rent.

Many also struggle to make mortgage payments
Hispanic/Latino homeowners also faced disproportionate pressure in making their mortgage payments. More than 12% of Hispanic/Latino Household Pulse respondents fell behind on mortgage payments at the start of the pandemic, compared to 7.6% overall. The same factors that contributed to difficulty making rent payments likely impacted the inability to make mortgage payments. For those who face housing insecurity as eviction moratoriums end, this may contribute to a further increased risk of exposure to COVID-19, if people are forced to leave their homes.

The insurance gap has widened
In April and May 2020, 15.94% of Hispanic/Latino people were uninsured, compared to 8.82% overall. This gap has continued to widen. According to the most recent household pulse survey, 15.15% of Hispanic/Latino people were uninsured compared to 7.25% overall.
Lack of insurance can compound other risk factors contributing to severe COVID-19. For example, those who lack health insurance are unlikely to seek treatment for chronic conditions like high blood pressure. Left unchecked, those conditions may lead to more severe expressions of the virus.

More Hispanic people know someone who has died from COVID-19
According to a March 2021 survey from the Associated Press and NORC at the University of Chicago, 29% of Hispanic respondents know someone who has died from COVID-19 compared to 19% of respondents overall. All the factors that lead to U.S. Latinos being disproportionally impacted by the virus have likely contributed to this higher chance of knowing someone who has died of the virus.
Some of these connections may be from workplace conditions that led to increased risk of exposure, such as working in grocery stores or meatpacking plants. Knowing someone who died of the virus made people report feeling more afraid of getting it themselves, making the high rates of economic and housing insecurity and lack of health care access in the Hispanic community particularly devastating.



