
This story originally appeared on Cognitive FX and was produced and distributed in partnership with Stacker Studio.
How COVID-19 affects the brain
A growing body of scientific evidence suggests some COVID-19 patients will experience neurological signs or symptoms of the infection. Genetic material from SARS-CoV-2, the virus that causes COVID-19, has been found in the cerebrospinal fluid of a person with COVID-19. And the virus has been found in the brain tissue of patients who died of COVID-19, which suggests it can affect the nervous system.
The frequency of symptoms appears to be associated with COVID-19 severity. In a study in China, patients with severe COVID-19 infection were more likely than those with nonsevere infection to have neurological symptoms of COVID-19, such as cerebrovascular disease, delirium, or musculoskeletal injury. Other neurological symptoms of COVID-19 include seizures and encephalitis.
The exact mechanisms by which SARS-CoV-2 affects the central and peripheral nervous systems is not clear. Neurological symptoms could be caused by the viral infection itself or be the result of other conditions such as sepsis, blood coagulation disorders, and vasculitis, which have all been reported in those with COVID-19. More research is needed, particularly as the number of people who have recovered from COVID-19 continues to grow.
Cognitive FX sought out information from scientific journals including The Lancet Psychiatry and the National Institutes of Health to put together a list of the six most common neurological symptoms associated with COVID-19 infection.
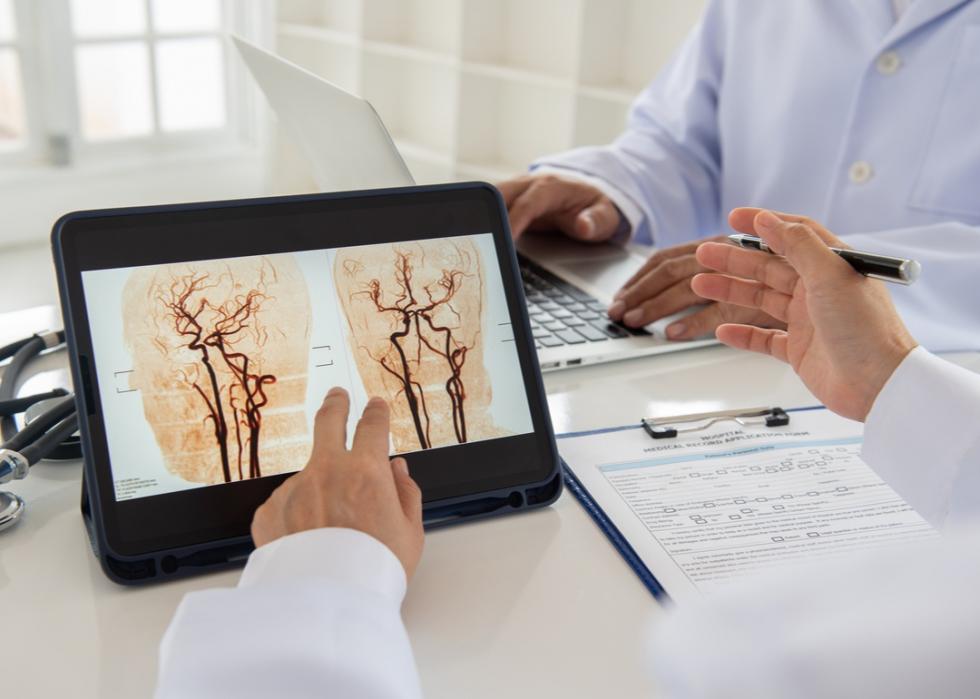
Cerebrovascular disorders
A 2020 study in The Lancet Psychiatry of almost 240,000 people with COVID-19 reported they had a little more than 2% rate of ischemic stroke. A subgroup of almost 9,000 people who were admitted to the intensive care unit had an almost 7% risk of ischemic stroke. In the same study, the rate of intracranial hemorrhage in those with COVID-19 was almost 1%, and the rate among those in the ICU was almost 3%. A small study in China reported that age, a history of diabetes or hypertension, severe COVID-19, and a significant inflammatory or coagulation response increased the risk of stroke in COVID-19 patients.

Anxiety disorder
A 2020 study that appeared in The Lancet Psychiatry reported that people diagnosed with COVID-19 had a more than 17% rate of anxiety disorder, and the rate among those admitted to the ICU with COVID-19 was greater than 19%. The researchers said the rate of psychiatric disorders such as mood and anxiety disorders was not as strongly associated with the severity of COVID-19 compared to the rate of neurological disorders, such as encephalopathy and stroke. This finding suggests anxiety disorder may reflect the psychological impact of a COVID-19 diagnosis, rather than being caused by the condition.
A review of 2020 research published in the international journal Acta Neurologica Belgica also found a relationship between COVID-19 and the onset of depressive conditions, especially in patients with severe cases of the virus.
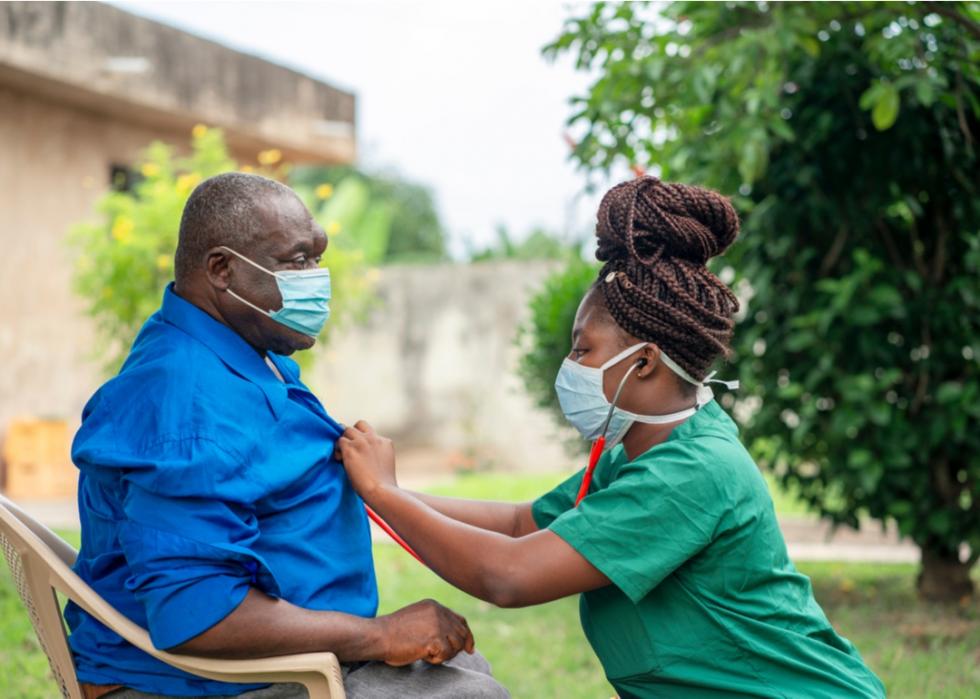
Dementia
The findings of The Lancet Psychiatry study support previous evidence of an association between COVID-19 and dementia. The more recent study reported that almost 3% of those over 65 had a first diagnosis of dementia six months after their COVID-19 diagnosis. Almost 5% of those with encephalopathy had a first diagnosis of dementia six months after diagnosis.
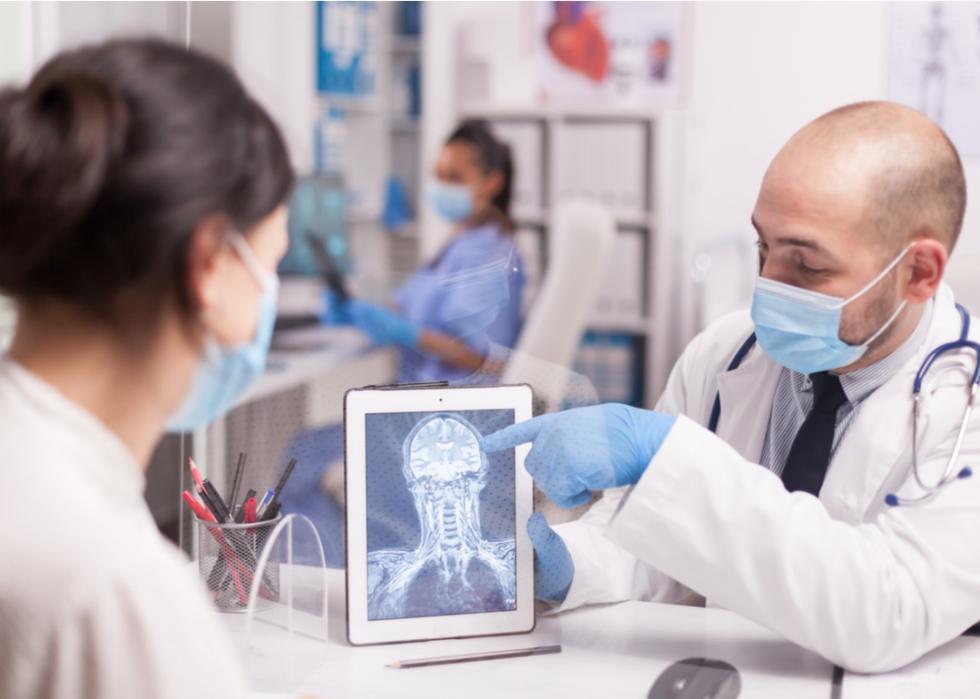
Encephalopathy
People with a history of severe respiratory distress and hypertension have an increased risk of developing encephalopathy as the first symptom of COVID-19. The risk increases with the severity of the infection. COVID-19-associated encephalopathy may have multiple causes, including metabolic factors; medication; and hypoxia, or insufficient oxygen. The symptoms of encephalopathy are treated with anticonvulsant medication; antipyretic, or fever-reducing medication; and high-flow nasal cannula support for oxygen therapy.
Encephalitis
Encephalitis, or inflammation of the brain, is a type of encephalopathy that is caused by an infection, including a viral infection. Symptoms of encephalitis include fever, headache, and delirium. Patients with COVID-19 may also have seizures. Those with COVID-19 may present with encephalitis rather than respiratory symptoms, although it is rare. A July 2020 study published in the journal Brain, Behavior, and Immunity suggests a link between COVID-19 and encephalitis.

Myopathy and neuromuscular disorders
A study of patients with COVID-19 reported that 44% to 70% of those hospitalized had myalgia and fatigue. Unfortunately, the rapid spread of the novel coronavirus prevented a thorough workup of COVID-19 patients that may have helped doctors determine how the infection caused these symptoms. Myalgia correlates with increased creatinine kinase level and lymphocyte count, which suggests COVID-19 may cause muscle damage and could interfere with muscle energy production, according to a study published in March 2021 by the International Journal of Clinical Practice.



