How to understand COVID-19 case counts, positivity rates, and other numbers
How to understand COVID-19 case counts, positivity rates, and other numbers
COVID-19 dashboards can serve as crucial resources for those following the pandemic. These dashboards pull statistics into one place and visualize the disease's impact over time. As fall starts, nine months into the COVID-19 pandemic, every state in the country and many major research institutions, news outlets, and volunteer efforts have developed pages devoted to tracking the outbreak. Some colleges, universities, and even school districts are getting in on the game.
The issue with COVID-19 dashboards is that they are inherently saturated with numbers. From case counts to death tolls, these statistics are arranged in a dizzying array of colorful tabs. It can be difficult to know where to click or what to read, much less how to take in all the data presented and understand how the pandemic is currently unfolding in your community. COVID-19 data have also become intensely political, as theorists on both sides of the aisle use numbers to advance their agenda rather than diving into what, exactly, the numbers mean.
Stacker consulted common COVID-19 sources such as the Centers for Disease Control and Prevention (CDC), the COVID Tracking Project, and the Council of State and Territorial Epidemiologists (CSTE) to compile a list of terms, principles, and data sources that can help you understand key COVID-19 numbers. Each slide provides context and information on where these numbers come from.
Read on to learn how to interpret your local COVID-19 dashboard and what data questions to ask at the next town meeting.
Editor's note: Betsy Ladyzhets is a volunteer with the COVID Tracking Project at The Atlantic, data from which was used for this piece.
COVID-19 case
A COVID-19 case refers to a person infected with the virus SARS-CoV-2 and is now sick with COVID-19. Cases may be symptomatic—meaning this individual exhibits common COVID-19 symptoms, such as a fever, cough, or shortness of breath—or asymptomatic, meaning they do not exhibit symptoms. It is important to include both types of cases in case counts to show where and how fast the virus is spreading.
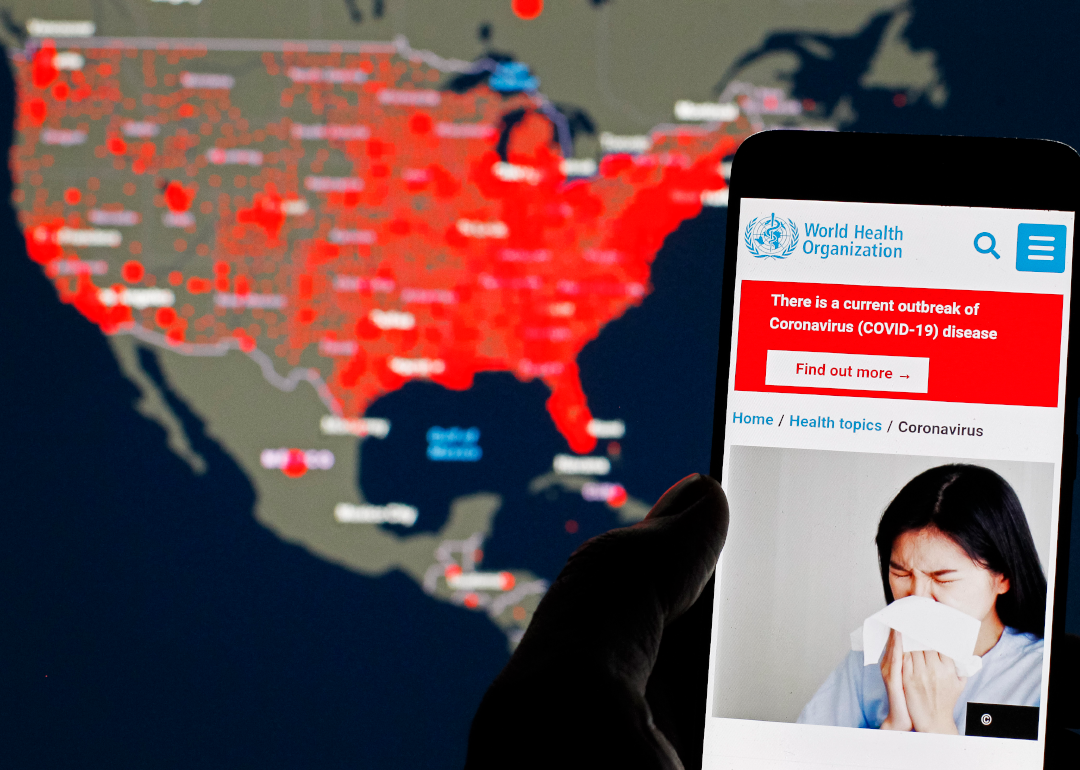
[Pictured: In this photo illustration the World Health Organization (WHO) Director General Tedros Adhanom Ghebreyesus is seen with a WHO coronavirus cases map displayed.]
Confirmed case
When a COVID-19 case is confirmed, this means that the infected individual has been diagnosed using an FDA-approved polymerase chain reaction (PCR) test. PCR tests work by searching for genetic material that matches the novel coronavirus in a sample of your mucus, saliva, or other material. These tests are highly accurate, which is why the Council of State and Territorial Epidemiologists (CSTE) considers them to be an effective test for identifying COVID-19 cases.
Probable case
A probable COVID-19 case, on the other hand, is identified through symptoms, exposure, or other types of tests that are less accurate than PCR. You may have a fever, chills, and a sore throat; you may have recently gotten lunch with a friend who tested positive for COVID-19 after you hung out; or you may have tested positive with an antibody or antigen test. But with any (or all) of these options, you would still need to take—and test positive on—a PCR test to be counted as a confirmed case of COVID-19.
Suspected case
A suspected case of COVID-19 is similar to a probable case, in that an individual is presumptively diagnosed based on symptoms or exposure to the virus but has not had their disease confirmed through PCR testing. Some public health agencies use the term "suspected" instead of probable to refer to hospital patients who have COVID-19 symptoms, but have not yet been tested or are awaiting test results.
Cumulative cases
A count of cumulative cases refers to all the people in a given region or institution who have been sick with COVID-19; such a count demonstrates how hard COVID-19 has hit a particular region or population. For example, according to the New York City public health department, 233,216 people in New York City have had the virus as of Sept. 12. That amounts to about 2.7% of all New Yorkers.
Daily cases
While cumulative case numbers reflect how many people in a given population have contracted the novel coronavirus overall, daily case numbers reflect how the coronavirus is progressing over time. Many public health agencies report daily cases on COVID-19 dashboards or in press briefings; they are often demonstrated in a line chart that makes it easy to compare today's number to yesterday's, last week's, and last month's.
Seven-day average cases
The problem with using daily case counts as a metric to track COVID-19 is that they often fluctuate due to factors unrelated to COVID-19 itself. Many laboratories—which process COVID-19 tests—and public health departments—which aggregate and report the results of those tests—do not work on weekends. This tends to cause fewer cases to be reported every Saturday and Sunday, while more cases are reported on Mondays to make up for the lag. As an example, check out Michigan's dashboard (daily cases tab): you can see drops in the new case numbers every weekend, and spikes at the start of each week. Significant amounts of new cases may also be added.
To account for this fluctuation, many researchers and reporters calculate a seven-day rolling average—the average of a particular day's new cases with the six days that came prior. This averaging practice smooths out daily peaks and falls into a trendline, which better reflects how cases are progressing over time. As ProPublica's Caroline Chen puts it: "It's kind of like the stock market; it's unhelpful to obsess over daily swings."
Active cases
Active cases refer to the individuals who both have been infected with the novel coronavirus and pose a risk to other people in their community. It's essentially the cumulative number of cases, minus those people who have either recovered from the disease, completed their time in quarantine, or passed away.
As many places in the U.S. do not have enough public health staff to keep track of how each COVID-positive person in their purview is doing, many states and counties cannot report active cases. However, this metric has become a popular figure on college and university COVID-19 dashboards, like this one from Carleton College, to let students know how many of their peers are currently sick and isolated on campus.
Transmission rate (R0)
R0, also called the transmission rate or reproduction number, is a figure calculated by epidemiologists to show how contagious an infectious disease is. The figure describes how a disease would spread in a kind-of vacuum if nobody in the population has been exposed to the disease yet, and there is no way to control its spread. If R0 is less than one, this means epidemiologists expect one person infected with the disease to spread it to less than one new person; if it is greater than one, each infected person will spread the disease to more than one new person. Scientists have yet to agree on an R0 figure for the novel coronavirus, as its progression through different populations is still under study.
PCR tests
Polymerase chain reaction (PCR) tests are the gold standard for diagnosing COVID-19. The tests are highly accurate because they identify whether genetic material matching the novel coronavirus is present in a person's body—akin to scanning your nose or throat for a super-specific barcode. PCR tests tell you whether you have the coronavirus right now, making them what scientists call diagnostic.
Antibody tests
While PCR tests tell you if you have the coronavirus right now, antibody tests tell you if you have had it in the past. These tests identify if your immune system has built up a response to the coronavirus by searching for antibodies, specific particles in your immune system that remember what a disease looks like, and help prevent you from getting sick with the same disease again. According to the CDC, it may take one to three weeks after a person is infected with the coronavirus for their body to produce an immune response and, as a result, for an antibody test to return a positive result.
As PCR and antibody tests measure different things and have different accuracy levels, it is important that any institution reporting them separates out the two numbers. For example, Texas reports about 5.5 million PCR tests and about 384,000 antibody tests as of Sept. 12. Of those Texans who took antibody tests, about 33,600 have tested positive; these individuals aren't included in Texas' case counts, since antibody tests cannot be used to diagnose a current case.
Antigen tests
Antigen tests, similar to PCR tests, tell you if you have the coronavirus right now. These tests are new—the FDA has approved only three types as of September—but they work more quickly and are cheaper to make than PCR tests, and some public health experts predict that they will be used widely across the U.S. by this winter. The tradeoff for this speed and cost-effectiveness is that antigen tests are not as accurate as PCR tests. If you take an antigen test and have it come back positive, you would still need to test positive on a PCR test to be diagnosed with COVID-19 officially.
Any institution reporting antigen tests should separate these counts from PCR tests, just as they should for antibody tests. But as of September, most states and the federal government are not reporting numbers of antigen tests conducted at all. The Atlantic's Alexis Madrigal and Robinson Meyer call this "dark testing"; without these counts, it is difficult to see a clear picture of COVID-19 testing in America.
False positive, test specificity
A false-positive test is one that has labeled someone as infected with the novel coronavirus, when in fact they have not contracted the virus. Such an error can lead to people facing unnecessary quarantines and restrictions, as well as extra work for contact tracers who are attempting to track the virus' spread in a community by talking to people who have tested positive.
When a test doesn't return many false-positive results, it is said to have a high specificity. This means that the majority of people who test positive do, in fact, have the disease. PCR tests have incredibly high specificity; if you tested positive, your result is very trustworthy. Antibody and antigen tests have lower specificities, which is why positive results with these tests must be confirmed through PCR testing.
False negative, test sensitivity
On the other hand, a false-negative test occurs when someone's test labels them as not infected with the coronavirus, when, in fact, they are infected. False negatives are dangerous because they can lead people to visit friends and family or go out into public spaces with a false belief that they are safe from spreading the virus to others.
When a test doesn't return many false-negative results, it is said to have a high sensitivity. PCR tests have a high sensitivity when performed correctly, while antibody and antigen tests have lower sensitivities. For example, an antigen test by manufacturer Quidel, the first to receive FDA approval, has an 80% sensitivity; one in five people who take this test could have false negatives.
Deduplication
Many test numbers reported by public health agencies undergo a deduplication process, involving the removal of doubled results from the count. For example, if you went to a clinic in your town to get tested last week, and then went back to the same clinic for another test this week, your name would appear twice in the list of people tested at that clinic. Your local public health agency might take your second test off their list of people tested—deduplicating your tests—so that you only appear on the list once.
Specimens tested
When you see a COVID-19 testing number reported by your local public health agency, school, or some other institution, it is important to ask what units this institution is using. Units refer to the magnitudes used to describe values; if you say the distance between your house and your office is three miles, "miles" would be the unit for that data point.
An institution that reports its COVID-19 tests in units of specimens is telling you the number of samples, taken from people's noses or throats, that were sent off to labs for testing. Multiple specimens may sometimes be taken from one individual—for example, if both sides of your nose are swabbed—so test counts reported in specimens may be somewhat higher than the actual number of people tested.
People tested
An institution that reports its COVID-19 tests in units of people is telling you the number of unique individuals who were tested. Arriving at a "people tested" number involves deduplication, as was explained on a previous slide; anyone in a particular region or institution who was tested multiple times or who had multiple samples taken during their test would be reduced to a count of one in the dataset. "People tested" numbers are useful for evaluating who has access to testing, but they are less helpful in assessing how many tests are conducted over time, as people who get tested several times would be removed from the dataset at each test after their first.
Testing encounters
Testing encounters are a new testing unit that allows for more accurate counts of test capacity over time. The COVID Tracking Project defines this unit as the number of people tested per day. This figure is not inflated by clinics that take multiple specimens from a patient, but it still includes multiple tests for people who are tested multiple times. As of mid-September, seven states are reporting testing encounters, according to the COVID Tracking Project.
Daily tests
Similar to daily cases, daily tests refer to the new COVID-19 tests conducted in a region or by an institution over a particular day. When looking at daily test numbers or testing time series, it is important to know in what unit these numbers are reported, so that you can interpret accurately. For example, Virginia reports testing encounters, allowing residents to examine a history of how many people have been tested in the state each day going back to March.
Test positivity rate
The test positivity rate is a calculated metric that shows what percentage of the tests conducted for a particular population has returned a positive result. This rate helps track test capacity over time. If a region has a lower test positivity rate, it likely means the region has testing available to all who need it and is more accurately diagnosing positive residents. Suppose a region has a higher test positivity rate. In that case, this likely means many people in this region are infected with the novel coronavirus. The region does not have enough testing available for its residents, and only people with symptoms are getting tested.
Similarly to examining units for test counts, when interpreting test positivity rates, it is crucial to examine units and ask for the underlying numbers behind the calculation: the total number of tests conducted and the number of those tests that were positive. In the past several months, some state public health agencies—and even the CDC itself—have artificially lowered test positivity rates by combining multiple test types in one number.
Test wait time
A test wait time, somewhat intuitively, refers to the length of time you wait between getting tested for COVID-19 and receiving your results. Ideally, test wait times should be two to three days if not shorter, allowing people who have been tested to act quickly to protect themselves and others while they are still symptomatic. Some potential COVID-19 patients have had to wait much longer this summer, however, due to lack of adequate testing supplies in states like Arizona and Texas. Reports on test wait times tend to be anecdotal; federal public health agencies and most states do not publish these numbers.
Current hospitalizations
Hospitalizations have become a useful metric for tracking COVID-19's impact on different regions and healthcare systems. The figure refers to the number of patients who are currently hospitalized due to severe cases of COVID-19. These patient counts may include only patients with confirmed cases of COVID-19 (identified through PCR testing), or they may include both confirmed and probable or suspected cases, depending on who is reporting the numbers.
Cumulative hospitalizations
A cumulative hospitalizations figure refers to the total number of people in a population who have been hospitalized due to severe cases of COVID-19. Similar to cumulative case counts, these figures are often not useful for tracking the pandemic's impact over time but can be used to identify demographic trends. For example, the CDC reports that Black Americans are 4.7 times more likely to be hospitalized for COVID-19 compared to white Americans, as of Aug. 18.
Hospital capacity
Keeping track of current hospitalizations for a given region, such as a state or county, allows researchers and public health leaders to calculate that region's hospital capacity: the share of available hospital beds which are currently occupied. The Department of Health and Human Services (HHS) reports hospital capacity estimates for every state, including the percent of all beds occupied (not COVID-specific), the percent of beds occupied by COVID-19 patients, and the percent of ICU beds occupied. These figures faced a great deal of public scrutiny after the HHS took over hospital data collection and reporting from the CDC.
Outcomes
Outcomes refer to the potential results of the disease. For COVID-19, these typically include death or recovery. COVID-19 patients who have underlying conditions such as diabetes and chronic kidney disease have an increased risk of more severe disease outcomes, meaning that their chances of hospitalization and death may be greater.
Recovered
When an individual infected with COVID-19 is included in a recovered count, it means that they are no longer considered to have symptoms or be in danger of spreading the virus to others. Many public health agencies report recovered figures, but definitions for how the figures are determined vary greatly; recovered cases may include specifically patients discharged from the hospital or include all COVID-19 cases that are no longer active. As a result, it's generally not possible to compare these numbers from state to state or across other jurisdictions.
COVID-19 death
The death toll of a disease is the ultimate way to track its impact on a population. However, more than any other metric, COVID-19 death tolls lag behind outbreaks in showing how badly a particular region has been hit, meaning that this number rises much later than others, such as cases and hospitalizations, as the disease progresses in vulnerable patients and these numbers are tallied. As a result, epidemiologists recommend watching case and hospital patient counts to see how your region is doing and watching death counts to see the final toll that COVID-19 has taken in your community.
Confirmed death
There are two ways that a public health agency may count COVID-19 deaths. The agency may track the outcomes of people who have confirmed cases, their infections confirmed by PCR testing. Alternatively, the agency may track the death certificates for its population and tally the certificates that list COVID-19 as a cause of death.
Confirmed deaths tend to refer to COVID-19 deaths identified through the first method: If someone receives a positive PCR test result, they become a COVID-19 case, and if they pass away while infected, they become a COVID-19 death.
Probable death
When COVID-19 deaths are tallied according to test results, a patient who did not receive a positive PCR test result but did receive a positive antibody or antigen test, exhibited symptoms of the disease, or had come into contact with an infected person, may be included in a count of probable deaths. Probable deaths may also include individuals for whom COVID-19 was a listed cause of death on their death certificate, depending on a particular public health agency's definition.
Excess deaths
COVID-19 has had a massive impact on America's population, with over 180,000 lives lost to the disease. But this number is likely far below the true number of lives lost: many Americans likely contracted COVID-19 but remained undiagnosed because of limited testing access, or died due to the immense impact this disease had on our health care system and economy.
One way to capture the scope of this true toll is by examining excess deaths, the number of deaths occurring in a particular window of time as compared to the number epidemiologists expect based on previous years. The CDC reports excess death estimates for every U.S. state; in some states, such as New Jersey, over 20% more people have died in February through September of this year compared to previous years.
Comorbidity
Comorbidity is an additional condition that contributes to a patient's death. In the case of COVID-19, some comorbidities, such as respiratory failure and sepsis, may be brought on by the coronavirus. Others, such as diabetes, hypertension, and Alzheimer's, may cause a patient's experience of the coronavirus to be more severe. While these conditions may play a role in worsening a patient's COVID-19 outcome, their deaths are still caused by the disease.
Demographic data
Presenting demographic data for a disease means breaking down case and death numbers according to different characteristics of a population, such as age, gender, race, and ethnicity. Analyzing such data is important because it can reveal disparities in how a disease is impacting different groups of people. For example, the Kaiser Family Foundation's analysis has demonstrated that people of color in America have less access to COVID-19 tests, but are at higher risk for both contracting and dying from the disease.
Long-term care facility
Nursing homes, assisted living facilities, and other forms of elder care are included in the blanket term long-term care facility. Such facilities have become a key area of study during the COVID-19 pandemic, as the disease has spread quickly through these homes for America's elderly population. As the COVID Tracking Project's Long-Term Care COVID Tracker reports: While residents in long-term care facilities make up less than 1% of America's population, they make up 42% of the country's COVID-19 deaths as of Sept. 10.
Looking at numbers in tandem
One common mistake that one may make while looking at COVID-19 data is analyzing one metric in isolation. For example, one cannot make a case that a region is recovering from its COVID-19 outbreak by looking at a declining death rate. Death rates tend to lag case rates, as mentioned on a previous slide—a region's death rate may be decreasing while more people become infected, and the case rate climbs back up. Instead, you must look at how much testing your region is doing, how many cases are identified through that testing, how your healthcare system is faring, and the outcomes of recent cases in order to see a complete picture of the pandemic's current impact on your community.
Put numbers in terms of people
COVID-19 numbers can often seem clinical when you're looking at a fancy dashboard full of color-coded charts and graphs. It can be challenging to remember that each value represents a person who has become sick or died from COVID-19. When reading a chart or a value in a news story, try to remember that the true units are American lives—and feel the urgency of reporting and understanding exactly what these numbers mean.
Recognizing uncertainty
All the COVID-19 numbers discussed in this story have some degree of uncertainty. Any given case count from a public health agency or other institution is likely missing people who were unable to get tested. Any test count might be combining values from different tests or conflating units. Any count of the lives lost may be missing many people who died due to the pandemic's impact but did not meet specific case definitions. And all this aside, many agencies have been figuring out how to report COVID-19 values as they do it, with new data reporting systems built and implemented along the way.
We will likely not know the true scope of what the pandemic has cost America for many years to come. The numbers that you see now are simply the best attempts of the smartest people working on this topic to capture what statistics they can right now.
[Pictured: Centers for Disease Control and Prevention (CDC) activated its Emergency Operations Center (EOC) to assist public health partners in responding to Covid-19.]
COVID Tracking Project
The COVID Tracking Project at The Atlantic is one such attempt to capture what statistics are available. The Project, an effort comprised of journalists, scientists, public health experts, students, and other volunteers, collects data on COVID-19 cases, testing, and outcomes from state public health departments and synthesizes those data for the public. It has become a trusted source for testing data, used everywhere from ProPublica to the White House. The Project releases daily tweets on the current state of COVID-19 data, as well as regular blog posts on trends and data issues.
Johns Hopkins
One of the first and most widely followed data trackers of the pandemic in the U.S. is managed by the Johns Hopkins University of Medicine. The tracker provides both global and U.S.-specific dashboards, which allow users to see case and death counts for regions as wide as the U.S. and as narrow as Los Angeles county. The Johns Hopkins tracker also provides resources on other aspects of the pandemic, such as testing and tracing, and articles that may help less scientifically minded readers understand the latest COVID-19 news.
[Pictured: The COVID-19 global cases map by the Center for Systems Science and Engineering (CSSE) at Johns Hopkins University (JHU) seen displayed on April 29, 2020.]
Department of Health and Human Services
The Department of Health and Human Services (HHS) is the federal government's primary source for COVID-19 data. You might not have heard of it before this pandemic, but it is actually an executive branch of the government which oversees the CDC, the National Institutes of Health (NIH), and other departments. The HHS has collected data on COVID-19 testing since U.S. testing began in February, and it has collected data on COVID-19 hospitalizations since it took over this collection from the CDC in July. Admiral Brett Giroir, the Assistant Secretary for Health under President Trump, currently serves as the country's COVID-19 testing czar.
[Pictured: Health and Human Services Secretary Alex Azar speaks during a press conference on January 28, 2020 in Washington DC. With Secretary Alex Azar is (from left to right) Centers for Disease Control and Prevention Director Robert Redfield, National Center for Immunization and Respiratory Diseases Director Nancy Messonnier, and National Institute of Allergy and Infectious Diseases Director Anthony Fauci.]
State and county dashboards
In many cases, the most reliable source for COVID-19 data is the most local source: your public health agency. You might look to the agency for your state, your county, or even your town to provide data and updates. Since these agencies have smaller spheres of people to monitor than federal public health departments, they can often quickly update values, notify their audiences when something goes wrong, and tailor their reports specifically for their communities. If you're not sure how to find your local agency, you might look to the COVID Tracking Project's sources, which list every state department.
Such agencies are also great places to direct questions about what a certain data point means or where the numbers are coming from. In this time of great uncertainty and confusion, asking questions—no matter how dumb they may seem—is the best practice you can develop for understanding COVID-19 data.