
As schools reopen, here's what we know about children and COVID-19
As schools reopen, here's what we know about children and COVID-19
Just nine days before New York City—the largest school district in the United States—was set to start its 2020-2021 school year, Mayor Bill de Blasio on Sept. 1 announced classes would be delayed to allow for further COVID-19 safety preparations. Children scheduled to go back to school in-person on Sept. 10 would not return until Sept. 21; most remote classes were similarly pushed back. The delay is part of a deal to avoid a teachers' strike in New York City and comes in the wake of protests and other expressions of concern by teachers and parents across the country. The U.S. is in a unique position that makes sending students back to school particularly daunting: We have the highest rates of COVID-19 in the world with nearly 6 million cases as of Sept. 1, according to the World Health Organization (WHO). Surging cases, high levels of community transmission, insufficient testing, and poor contract tracing in the U.S. make it difficult to compare school reopenings with countries where the virus is more controlled.
There are still unknowns about how COVID-19 impacts children, but a growing body of studies shed some light. Children who contract COVID-19 are more likely to show mild symptoms or no symptoms at all, though a very small number have come down with Multisystem Inflammatory Syndrome (MIS-C), a rare COVID-19-related condition doctors don't yet fully understand. It's also unclear if children are less likely to be infected and whether, once infected, they transmit COVID-19 at the same levels as adults.
While researchers fill in the gaps of our knowledge, some concrete facts about children and COVID-19 have emerged. Stacker compiled a review of facts and statistics about how COVID-19 relates to children in the U.S. from the Kaiser Family Foundation (KFF), the Centers for Disease Control and Prevention (CDC), and other public health sources. For the purposes of these statistics, children are considered to be anyone in the population younger than 18.
You may also like: Debunking COVID-19 myths

Children account for 8% of COVID-19 cases in the US
Children 17 and younger account for 8.1% of reported COVID-19 cases as of Sept. 1. Children 4 and younger comprise 1.7% of cases, while those between the ages of 5 and 17 make up 6.4% of cases, pointing to an age gradient of susceptibility to the disease.

Over 476,000 children have tested positive for COVID-19
While children make up less than 10% of America's COVID-19 cases, the number of infected kids is still high. A study by the American Academy of Pediatrics which compiled data from state public health departments found an overall rate of 631 COVID-19 cases per 100,000 children in the population, as of Aug. 27.

Children account for 1% of reported COVID-19 hospitalizations in the US
Children account for about 1.5% of COVID-19 hospitalizations as of Aug. 22, demonstrating that most infected children experience less-severe COVID-19 symptoms than adults. Milder symptoms—or no symptoms at all—mean children don’t require medical intervention at the rates of adults.

Children account for under 1% of reported COVID-19 deaths in the US
Children are 22% of the U.S. population but make up less than 1% of the country’s deaths. Both age ranges reported by the CDC—ages 0 to 4 and 5 to17—represent less than 0.1% of all COVID-19 deaths.

Over 90% of children with COVID-19 have no or mild symptoms
An expert panel in July reported that, of children who contract COVID-19, more than 90% will have no symptoms or mild symptoms. Those who do have symptoms are likely to experience mild upper respiratory issues in the nose, sinus, and throat—as opposed to adults who often also suffer lower respiratory symptoms of the lungs.
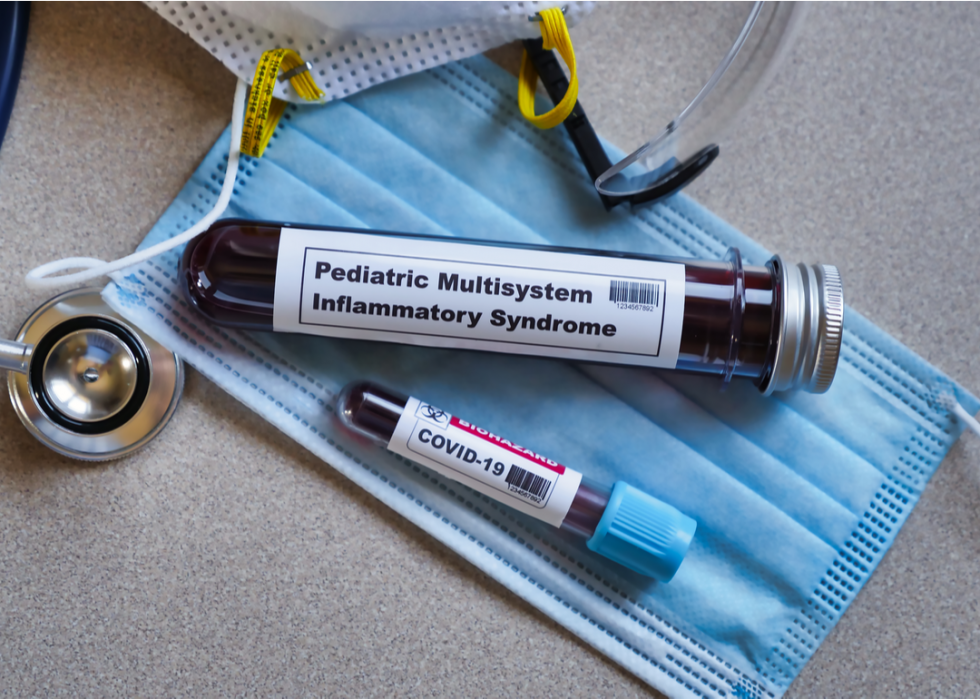
694 children in the US have contracted Multisystem Inflammatory Syndrome
Multisystem Inflammatory Syndrome (MIS-C) is a rare condition that is still not fully understood. There have been 694 cases reported as of Aug. 20. Most children have recovered, but there are 11 reported deaths. Some children develop the syndrome weeks after contracting COVID-19, but others have developed MIS-C seemingly without having a prior COVID-19 infection.

Children under 10 are less susceptible to infection
There is early evidence that children younger than 10 are significantly less susceptible to infection than adults when experiencing the same exposure to COVID-19. This supports findings that showed the virus didn’t spread as much in elementary schools compared with middle and high schools last spring.

Older children may be infected at rates similar to adults
While children younger than 10 are less susceptible to infection, older children may be at the same risk level as adults. More evidence is needed, as there are currently competing studies: One published in Nature Medicine in June shows 20 years of age may be the cut-off point, with those younger than 20 having about half the susceptibility to infection as those older than 20 years. A different study, however, showed children over 10 years of age as having infection rates similar to adults.

Adults are more likely to infect children than the other way around
While experts aren’t sure if children transmit the virus at the same rates as adults, several studies have found that a majority of COVID-19 transmissions between children and adults occurred from adults to children, and not from children to adults. Young children in particular are less likely to be the source of infection in households where people test positive for COVID-19.
Children are less likely to be tested for COVID-19
Children are less likely to be tested for the virus for a few key reasons, including the fact that testing in the U.S. has focused mostly on symptomatic patients with more severe symptoms. Kids are more likely to be asymptomatic or have less severe symptoms if they do appear to have contracted COVID-19. The lack of testing means the data of how children are impacted by the virus is also lacking.

Children may be left out of contact tracing investigations
Since kids are less likely to show COVID-19 symptoms, they are often not identified as the “index” case (the first in a group of linked cases, or, patient zero) in contract tracing efforts. The Kaiser Family Foundation reports this could mean the role children play in transmission of the virus could be “underrecognized.”

The CDC recommends face coverings for children 2 years and older
As difficult as it may be to make a toddler properly wear a face mask, the CDC recommends face coverings for kids 2 years and older. Masks should be worn in public spaces where it is challenging to practice social distancing and should cover their mouth and nose.

Children should practice everyday preventative behaviors just like adults
In addition to wearing face masks, the CDC says children should practice all the same preventative practices as adults. This means keeping a distance of 6 feet or more between kids and other people, despite how difficult that may be to enforce with younger children. Parents and caregivers should also try to disinfect high-touch surfaces in high-traffic areas every day, wash toys (including plush ones) when possible, and encourage thorough and frequent handwashing.

Outdoor activities are safer for children
It’s always beneficial to encourage children to spend time outside—that may be even more true during the pandemic. The CDC suggests infrequent playdates held outdoors still pose a medium risk of COVID-19, but it is preferable to indoor playdates with less ventilation where it’s also more difficult to ensure social distancing between kids.

Children should avoid visiting older family members if possible
It is well documented that older people are at higher risk of more severe cases of COVID-19 and health officials highly recommend that high-risk people limit contact with children. While this poses extra challenges for parents who rely on grandparents for childcare—and multigenerational households—the fact that children are more likely to be asymptomatic makes this guideline all the more vital.

Statewide school closures in spring 2020 were associated with decreased COVID-19 cases and deaths
The decision to close schools was a controversial one, but a study published July 29 in the Journal of the American Medical Association found over a period of 26 days, there could have been 424 more infections and 13 more deaths per 100,000 people had schools not decided to close. The study’s authors note that this connection does not prove cause and effect, but it does illustrate a connection between school closures and reduced case counts.

Schools may be safely reopened if community transmission is low
In countries that successfully slowed the spread and control of outbreaks—like South Korea, Finland, New Zealand, and Vietnam—school reopenings did not result in new outbreaks. This is because those countries have low levels of community transmission. The U.S., meanwhile, has comparatively much higher levels of community transmission.

Major outbreaks have been associated with school reopening in some countries
Some countries, however, did experience new outbreaks when schools reopened. Canada, Chile, France, and Israel reported outbreaks when children returned to schools. In the case of Israel, which reopened schools with few mitigating measures such as distancing and masks, school-based cases were high enough to increase community transmission.

3.3 million seniors live in households with school-age children
About 6% of senior citizens live in homes with school-age children, exacerbating the already complex issue of safely reopening schools. While children have proven to be statistically less infected by COVID-19 and do not represent chief means of transmission in communities, there is the potential for a child to contract COVID-19 at school and transmit it at home to a family member.

Nearly 1.5 million teachers are vulnerable to serious illness if infected with COVID-19
While children are infected and hospitalized at significantly lower rates than adults, school reopening must still take into account the adults who work in the buildings. Of the teachers and other instructors in the U.S., one in four have a condition that puts them at elevated risk for serious illness should they contract COVID-19. That's 1.47 million people who are potentially at risk by returning to schools to work.

Rate of COVID-19 in children steadily increasing
A CDC briefing from August 2020 for pediatric healthcare providers reported that the rate of COVID-19 cases among American children has been "steadily increasing" from March to July 2020. The CDC noted that, while children still comprise a small fraction of U.S. cases, lack of widespread testing for kids and the prioritization of testing those with severe symptoms has likely led to underreporting.

Over 4,000 cases connected to US schools
A crowdsourced tracking project started by Kansas high school teacher Alisha Morris and now monitored by the National Education Association found that 1,081 K-12 schools in the U.S. have seen 4,282 cases and 75 deaths since March 1. These figures reflect cases and deaths reported in news outlets, and likely reflect a significant undercount of the impact schools have had on America's COVID-19 outbreaks thus far.



