
What you need to know about how COVID-19 spreads through air
What you need to know about how COVID-19 spreads through air
Since the first cases of COVID-19 in Wuhan, China, in December 2019, scientists and others have been playing a constant game of catch up, trying to figure out in real time how the virus spreads and what are the best ways to prevent transmission. Now, more than 10 months later, as a global milestone of over 40 million documented infections is reached, scientists have much more information about how the virus moves through the air and infects others.
Scientists now believe that the three main forms of transmission of SARS-CoV-2, the virus that causes COVID-19, are droplets; aerosols; and fomites, or surfaces. This increased understanding has led to a scientific consensus about the importance of wearing masks and also reinforces recommendations that have been made since the beginning of the year of consistent hand-washing and keeping distance from one another.
In order to better understand what concrete steps should be taken in light of these most likely transmission pathways, a group of scientists and engineers with research experience in aerosols and air quality compiled a report titled "FAQs on Protecting Yourself From COVID-19 Aerosol Transmission." A full list of authors is available on the fourth page of the report, which explains the best types of masks to wear, the safest activities to partake in and how aerosols spread, among other important information.
Stacker consulted this report and compiled the 50 most important things to know about how COVID-19 spreads through the air. It has used version 1.78 of this report, which was published on Oct. 1, 2020. As information about COVID-19 is complicated and ongoing, it is important to always look for the latest information from reliable sources. Given the information that is currently agreed on by scientists, the following can offer some helpful information to help you make the safest choices during this pandemic.

COVID-19 spread through large droplets
One of the main methods of transmission of Sars-COV-2, the virus that causes COVID-19, is through large droplets, which are particles of saliva or other respiratory fluid that are expelled from individuals when they cough or sneeze or occasionally just through talking. When these droplets are expelled by an infected person, they fly like a projectile through the air, hitting other people on their mouths, nostrils, or eyes. When there is no one for these droplets to hit, they fall to the ground within a 3- to 6-foot radius.

COVID-19 spread through aerosols
Along with larger droplets, COVID-19 also spreads through aerosols. These are particles of saliva or respiratory fluid that are smaller than roughly 100 micrometers and can linger longer in the air, sometimes for hours. They can also travel longer distances due to their small size. They infect people by being inhaled through the nose or mouth or in rare cases, by deposition on the eyes.

Size distinction between droplets and aerosols
The difference between droplets and aerosols comes down to size. Particles smaller than around 100 micrometers are aerosols and are able to travel further and linger longer in the air. Larger particles are considered droplets. Droplets larger than around 300 micrometers have enough force to reach someone else at 0.5-1 meter, or approximately 3 feet, roughly the distance people stand from one another when having a conversation. Between 100 and 300 micrometers, particles typically are unable to infect others as they are too large to linger like aerosols, but too small to move as ballistic droplets and reach others.

Secondhand smoke as an analogy for aerosols
When thinking about the spread of aerosols, it can be helpful to use secondhand smoke as an analogy. Like secondhand smoke, aerosols do not fall to the ground quickly and are most concentrated in front of the person who expelled them, then mixing in the air currents and building up in rooms with low ventilation. In most indoor environments, less than 10% of the aerosols will deposit onto indoor materials and the rest will stay airborne until released to the outdoor air.

Most common form of COVID-19 spread
Scientists are still debating the most common form of COVID-19 spread. The most recent CDC guidance says that the droplet is the principle mode, that aerosols also play a role, and that fomites play a more minor role. However, this information could change.

Different people have different contagious levels
Different people have different levels of contagion at different times. Peak contagiousness happens just before and at the onset of symptoms, and then the contagiousness decreases. By the time people are sick enough to go to the hospital, many are no longer contagious. And virus emission, or shedding, is not necessarily a constant event but rather sporadic. In addition, some individuals are likely more contagious than others due to higher viral load at the onset of symptoms, higher emissions of particles, or both. Some people exhale up to 10 times more aerosols when speaking.

Superspreader events
The very high rate of spread of SARS-CoV-2 at certain large events can only be explained by airborne aerosols. The likelihood of an event becoming a superspreader depends on the activities attendees are participating in, such as loud talking or singing for example, and the ventilation in the space. This leads to a skewed distribution of R0 values, the rate of spread, because there can be very low or high values depending on specific situations.

Size of infectious aerosols
The size of the SARS-CoV-2 virus itself is very small, around 0.12 microns. However, the aerosols in which these viruses are contained are larger, which has implications for the ability of masks and filters to remove it from the air, for how deeply it will enter into the lungs and how long they will stay in the air, making them more likely to be inhaled by others.

How infectious aerosols are exhaled
The size of aerosols and amount of virus exhaled vary from person to person and is based on an individual’s stage of infection. They also vary based on the activity being undertaken, for example, talking, singing or shouting can lead to more aerosol exhalation. Aerosols can stay floating in the air for minutes and sometimes up to hours. If another person enters the space and inhales them, they can become infected and go on to infect others.

Where aerosols enter the respiratory system
Coming back to the smoke analogy, aerosols operate in a similar fashion. When aerosols are inhaled, some deposit in the respiratory tract and some are exhaled back out, like smoke. The aerosols that are around the size of 0.3 micrometers are more likely to be exhaled back out, so even though masks are not very efficient at blocking such small aerosols, those same aerosols are less likely to stay in our respiratory tracts.

How long the coronavirus stays infectious in aerosols
There have been multiple laboratory studies looking at how long SARS-CoV-2 stays infectious in aerosols. Overall, they have found that at typical room temperature (about 20 Celsius or 70 Fahrenheit), the virus’ lifetime is around one or two hours. This means that people at high risk are better off going to indoor public spaces as soon as possible in the morning, because any virus from the day before will be gone, whereas once a space has been open for a couple of hours, there could be lingering viral aerosols.

How temperature impacts virus survival
The virus survives better in lower temperatures than in higher ones, and researchers freeze viruses when they need to keep them viable for years. This could explain superspreading events in meatpacking plants, where temperatures are kept low.

How humidity impacts virus survival
Viruses in lipid envelopes, such as SARS-CoV-2, are believed to survive better in the air in less humid conditions. In addition, drier conditions are also thought to make humans more susceptible to viruses because it is more difficult to clear mucus and increased tissue damage.

COVID-19 and smoking
Smoking can increase viral transmission into the air. This is not due to the smoke itself, rather it is due to the fact that smokers must remove their masks in order to smoke and because their smoking habit may cause them to breathe more forcefully. However, because smoking and vaping destroy cilia in the respiratory tract, which are home to the ACE2 receptors that viruses use for infection, smokers have been observed to be less likely to be infected by COVID-19, but if they are infected, they could be at risk for more severe illness.

COVID-19 and pollution
Pollution aerosols are much smaller than the aerosols that dominate SARS-CoV-2 transmission, about 0.3 micrometers compared to 3 micrometers. So far, there has been no evidence to show that pollution aerosols do anything to enhance transmission of SARS-CoV-2. Like smoking however, it is likely that people in highly polluted areas could experience worse outcomes if they are infected due to having already vulnerable respiratory systems from pollution.

Close proximity infection
COVID-19 transmission often takes place in close proximity situations, meaning being within 2 feet of another person. However, as shown from contact tracing, not all close proximity situations lead to infection.

Shared room infection
As superspreading events have shown, there is clearly aerosol transmission of SARS-CoV-2 in public and shared indoor rooms. This superspreading is most likely to take place when people are in these places for a long time, when there is crowding, poor ventilation, no masks, and people are talking, singing, or yelling. This means lots of outbreaks occur in bars, meatpacking plants, and choirs, but no known outbreaks have been reported in Japan’s crowded subways or in movie theaters, places with less talking and better ventilation.

Long-range infection
There are no known documented cases where transmission of COVID-19 takes place over long distances through aerosols. The only long-range transmissions that have been documented took place in feces through the sewer lines of high-rise buildings in China and Hong Kong.

6-foot rule
Keeping a “social distance” of 6 feet will reduce, but not eliminate, the risk of spread. The 6-foot rule is based on the fact that large ballistic droplets fall to the ground within 6 feet, although they can travel farther with a cough or sneeze. With aerosols, the 6-foot rule can also apply because aerosols generally hang in the air close to where they were released, similar to cigarette smoke. The aerosols are diluted as they travel further distances, which is why social distancing tends to be relatively effective, although not foolproof.

Timing of inhaling infectious aerosols
There is no exact amount of time that is safe to spend in close proximity or in a shared room with someone who is infected, but it is likely in the order of minutes, not hours. The CDC uses 15 minutes as its threshold for how long is typically needed to become infected. However, this is not supported by specific evidence and can give a false sense of security.

How long the virus stays in indoor air
How long the virus stays in the air with the ability to infect others depends on the size of the droplet or aerosol carrying the virus, and the amount of clutter and air circulation in the room. Air circulation is especially important as the faster infected air can leave a room, the less likely it is to infect others. When outdoor air enters an indoor space, it mixes with the indoor air and replaces it. In residences, 95% of the indoor air will likely be replaced with outdoor air in as little as 30 minutes or as much as 10 hours. In public buildings, that time is between 12 minutes to 2 hours, and in a hospital, 95% replacement can happen in as little as 5 minutes.

Protection from indoor aerosol transmission
A person can never be completely safe from transmission of the virus, but there are steps one can take to reduce the risk. These steps include trying to reduce situations where one would be inhaling the air of others, such as being in crowded spaces, being close to others, being in environments with poor ventilation, being around people without masks, and being around others indoors for a long time.

How masks reduce aerosol spread
Surgical masks are able to stop smaller particles like aerosols because even though the holes of the mask may be larger than the particles, the particles get stuck on the mask material, like a fly on a spiderweb. Even other types of masks, like cloth masks, do a good job because when a porous obstacle is put in the path of aerosols, then at least some of them will end up caught in the obstacle.

Choosing a mask
A mask’s effectiveness against transmission of the virus depends on two factors: how well the mask fits and if the material it’s made of is effective at filtering out aerosols of different sizes. An N95 mask that fits properly can keep out at least 95% of any size of aerosol for the wearer. Surgical masks offer 70-80% protection. Cloth masks with pockets that hold filters are also effective. And studies have found that homemade masks made out of single layers of cotton or other material offer around 50% protection. Using two layers or more of fabric in a mask can increase protection to 90%.

When to wear a mask outside
Masks should be worn outside if you are regularly passing others at a close physical distance. If you are able to maintain space from others or are outside in places where you are not in contact with other people, then masks are not as important outside.

Mask over the nose
It is very important to wear your mask over your nose along with your mouth. Aerosols also come out of your nose when you exhale and are inhaled through your nose as well.

Fit of a mask
The fit of your mask is very important to protect against aerosols, because gaps will allow air to flow through. When your mask fits well, the material should suck up against your mouth and nose when you inhale.

Removing a mask to talk
Talking results in roughly 10 times more respiratory aerosol emission than just breathing. Therefore, masks should be kept on when talking, unless you are outdoors at a sufficient distance from another person.

Eye protection
Eyes are thought to be a possible, but not very important, route of transmission for aerosols because much more air is taken in by the lungs than could hit the eyes. More likely is if someone coughed or sneezed toward you, the ballistic droplets from that could impact the eyes, or hit your fingers, which you might then put in your eyes. Regular glasses are protective against ballistic droplets and safety glasses are better for aerosols.

Face shields
While face shields might look effective, they do not offer much protection against aerosols. They are better at protecting the wearer from ballistic droplets instead. They can be considered as a good addition to masks for eye protection, but they are less useful than closed glasses, and not a substitute for a mask.

Plexiglass barriers
Plexiglass barriers are most effective for avoiding direct droplet and aerosol transmission when distance cannot be maintained between people. However, because aerosols move with the air indoors, plexiglass barriers are less effective against aerosol transmission.

Outdoor aerosol transmission
Data shows that being outdoors is much safer than being indoors when it comes to virus transmission, all other factors being equal. However, nothing is 100% safe. Being in crowded locations or in more confined spaces with low wind conditions and away from the sun—because ultraviolet (UV) rays work to deactivate the virus—are riskier conditions.

UV sunlight kills the coronavirus
UV light from the sun is effective at deactivating the virus, especially at high intensity. At a UV index of 2, the virus can survive for around 1 hour. In full sun and a UV index of 10, that survival time goes down to only 10 minutes. This is most important for the virus on surfaces, which will be deactivated much more quickly if left outside during the day.

Outdoor dining safety
It is much safer dining outdoors than indoors, but it is still important to maintain distance between tables and wear a mask when not actively eating or drinking. It is best to avoid tables downwind of other tables. When interacting with the server, both you and the server should be wearing masks, and people who are not already living together should not sit at the same table, because the virus transmits best at close proximity when talking.

Outdoor recreation safety
Outdoor recreation is a low-risk activity as long as people are able to maintain distance or people wear masks when they are not. The virus is not known to be transmitted through water.

Taxi cab and ride-share safety
To take a taxi cab or ride-share safely, it is important that both customer and driver wear a mask. It is also preferable to have two windows at least partially open during the trip, and if ventilation is used within the car, make sure that it is set to outside air and not recirculated air, which would keep aerosols moving throughout the car. Shorter trips are better to reduce exposure time.

Public transportation safety
Public transportation has so far experienced no known superspreader events. Public health experts say taking mass transit is less safe than walking outdoors, but safer than indoor dining. Many transit agencies have adopted mask mandates, and cleaning the subways and buses frequently.

Airplane safety
Modern, large airplanes have good ventilation and air filtering systems, so the biggest risk for COVID-19 on a flight would come from the people next to you. As with other indoor activities, this risk can be reduced by wearing a mask and talking less. This is especially important during boarding and deplaning, when there is less ventilation. Smaller airplanes also may have poorer ventilation.

School safety
Schools unfortunately have a lot of the features that help spread the virus: they are indoors; have poor ventilation; students are close together; can be crowded; and children often talk, yell, and sing. There is still much debate and uncertainty about how well children transmit the disease, with some evidence that young children are less-effective spreaders, but schools should be modified to reduce the risk of spread.
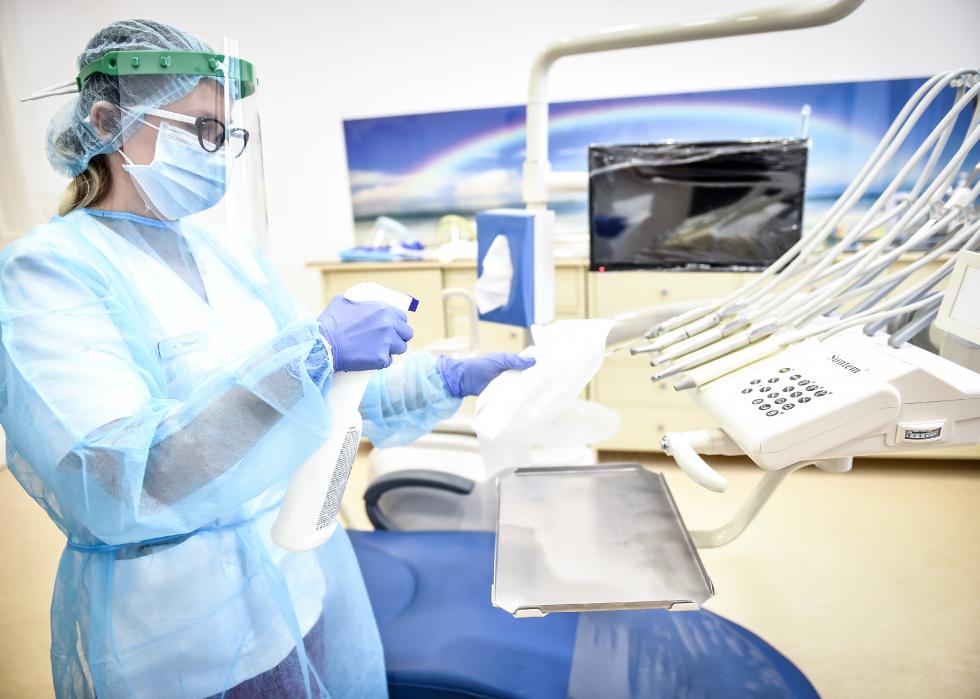
Dental office safety
Dentists may be at high risk of infection by patients because aerosols are generated at high rates during dental procedures. There is also risk to the patient, especially if the dentist's mask is not of high quality or does not fit well. In dentistry, some of the aerosols can be removed at the source by extracting air near the mouth. This is still not fully investigated.

Elevator safety
Modern elevators tend to be well-ventilated with air exchange rates of up to one per minute during travel, plus additional air exchange when the doors open. The primary concern of elevators, like all indoor spaces, is being in close proximity to others. Masks should be worn and talking should be limited.

Public bathroom safety
SARS-CoV-2 is found in feces but does not seem to be infectious in that format. However, it can potentially spread through aerosols when the toilet is flushed, so it’s a good idea to close the lid when flushing. It can also potentially spread through plumbing systems in high-rise buildings where there are bathroom floor drains, which are not common in the United States, that can bring air contaminated with fecal aerosols into a person’s bathroom.

Safety for musicians
Singing generates aerosols and numerous COVID-19 outbreaks have been linked to large groups of people singing together in places with poor ventilation for an extended time period. A recent yodelling concert in Switzerland is believed to have become a superspreader event. There is ongoing research on wind and brass instruments, and it’s been shown that instruments that need back pressure to generate sound—such as oboes, clarinets, and trumpets—spread more aerosols. It’s recommended to play wearing a mask with a slit for air, to practice for 30 minutes or fewer indoors, and to have a good air filter. It is preferable to play outside.

Ventilation
Ventilation means diluting indoor air with outdoor air, which is important because this could potentially dilute air with the virus with air without the virus. Opening windows is the most basic method to increase ventilation. Installing fans in windows helps move even more air. And fans should also blow out the window, so that any air with the virus will be pushed out of the room.

Air filters
Air filters should effectively remove particles around 10 micrometers or smaller, which includes most respiratory aerosol particles. Filters therefore help to reduce virus-containing aerosol concentrations and standard filters should be upgraded if possible.

Portable air cleaners
Portable air cleaners that use filtration can be effective because they can reduce the concentration of virus-relevant aerosol sizes. A side benefit of this filtration is that allergens and pollutants can also be decreased.

Controlling heat and humidity indoors
As stated earlier, SARS-CoV-2 survives better in drier conditions and therefore, in theory, dehumidifiers can help reduce the virus’s survival time. However, ventilation and filtration are simpler and more efficient. Dehumidifying alone does not physically remove the virus from the air, although it does make it decay more quickly.

Relative risk for different environments
Different locations have different risk levels for the spread of COVID-19. National Geographic adapted the aerosol transmission estimator into an online calculator to give visual estimations of the different risks of different situations. For example, an indoor gathering with talking in a poorly ventilated space is much riskier than riding the subway or attending a lecture in a classroom.

COVID-19 spread through surfaces
There has been much concern about the spread of COVID-19 through surfaces as well, which is why everyone is told to wash or disinfect their hands frequently. This is known as the fomite path, and comes from touching a surface with SARS-CoV-2 such as a light switch, door handle, or someone else’s hand. Once the virus transfers to your hand, you can infect yourself by touching your mouth, nose, or eyes.

Protection from surface transmission
As of the writing of this guide, it is understood that aerosol transmission is more likely and therefore more important to mitigate than fomite transmission. However, fomite transmission is still possible so it is important to continue washing your hands and using sanitizer, but the air you breathe deserves at least as much, if not more, attention.



