How vaccines get made and approved in the US
How vaccines get made and approved in the US
On Dec. 11, Pfizer's COVID-19 vaccine became the first to receive authorization for distribution in the U.S. Members of a special U.S. Food & Drug Administration (FDA) committee that advises the organization on vaccines met the previous day to discuss data from Pfizer and its partner BioNTech. The Pfizer and BioNTech vaccine has demonstrated 95% efficacy in its clinical trial and was praised by FDA scientists upon their review of the trial's detailed scientific results. At the end of the Dec. 10 meeting, the committee voted that the Pfizer vaccine is safe and should be given emergency authorization by the FDA. The agency itself granted this authorization the next day.
One week later, Moderna followed Pfizer: the FDA advisory committee met, discussed data from the clinical trial for Moderna's vaccine (which has demonstrated 94% efficacy), and recommended that the agency authorize distribution of this product. The FDA is expected to again follow its committee's recommendation within days. The nation watched as an initial group of doctors and other hospital staff got Pfizer shots starting on Dec. 14; Moderna's vaccine may be close behind in protecting health care workers and other vulnerable populations.
COVID-19 and its wide-ranging impacts on the lives of nearly everyone on the planet have brought vaccines to the forefront—if enough suitable vaccines can be created, produced, and widely distributed, then life could perhaps resume some semblance of normalcy. People around the world are waiting impatiently for news of vaccine authorization and distribution, looking forward to a better 2021.
However, there is also mistrust surrounding vaccines, and often a lack of understanding about how they are created, how they are tested, and how safe they are. If people don't trust the vaccine, then people won't take it, and the pandemic could go on longer.
Some of this lack of trust comes from a lack of information and misinformation. In order to demystify vaccines and the vaccine manufacturing and approval process in the United States, Stacker consulted the FDA, Centers for Disease Control and Prevention (CDC), and other public health sources to better understand and explain vaccines to the general public.
After going through these authoritative health information sources, Stacker identified some key terms to help readers better understand the types of vaccines and how they work, and then listed the many steps involved in the creation, approval, and distribution of new vaccines in the U.S. We then created a list of 30 key terms and steps, showing how intensive and precise the vaccine creation and approval process is, and ultimately that vaccines are safe and effective tools for fighting disease.
You may also like: States with the highest COVID-19 infection rates

U.S. Food & Drug Administration (FDA)
The U.S. Food and Drug Administration (FDA) protects public health by ensuring the efficacy and safety of biological products, including food and drugs such as vaccines. This means that for any vaccine to be approved for distribution to the American public, it must first be approved by the FDA.

Center for Biologics Evaluation and Research
The specific area of the FDA that deals with vaccines is the Center for Biologics Evaluation Research (CBER). This center regulates biological products using an array of regulatory measures, such as the Public Health Service Act and the Food Drug and Cosmetic Act.

Identifying an antigen
The process to create a vaccine is historically a long one. It begins with scientists and researchers identifying the antigen, which is the part of a germ that the immune system can recognize and attack to prevent the targeted disease.
Stimulating the immune system
Vaccines work by stimulating a reaction from the immune system. They do this by essentially tricking the body into thinking there’s an infection. While the body may occasionally experience minor symptoms of infection after getting a vaccine, the kind of pseudo-infection introduced by the vaccine almost never causes illness.

Whole-pathogen vaccines
Whole-pathogen vaccines are the traditional type of vaccine. These vaccines contain entire pathogens that have either been killed or weakened enough that they cannot cause disease. Because they have whole pathogens, they elicit strong immune responses. However, not every disease can be targeted with this type of vaccine.
Subunit vaccines
Unlike a whole pathogen vaccine, a subunit vaccine uses just the antigens to best stimulate the immune system. This vaccine design is safer and easier to produce, but it often requires the addition of adjuvants, components that elicit a stronger immune response, because the antigens are not sufficient on their own for long-term immunity.
Nucleic acid vaccines
Nucleic acid vaccines use genetic material to encode the antigen or antigens needed to produce an immune response from the body. This allows the body’s own cells to produce the antigen(s) using the genetic material. The advantages to this type of vaccine are long-term immune responses, scalability, and vaccine stability. Some of these vaccines are based on mRNA (messenger DNA). Both the Pfizer/BioNTech and Moderna coronavirus vaccines use mRNA.

Multiple-dose vaccines
Some vaccines require more than one dose. There are a few reasons for this. Some vaccines do not provide much immunity in the first dose, and therefore need more. In others, immunity wears off after time, and “booster” doses are needed. In some live vaccines, multiple doses make it more effective. And in the case of the flu vaccine, a new dose is needed every year because the flu virus that causes the disease varies year to year.
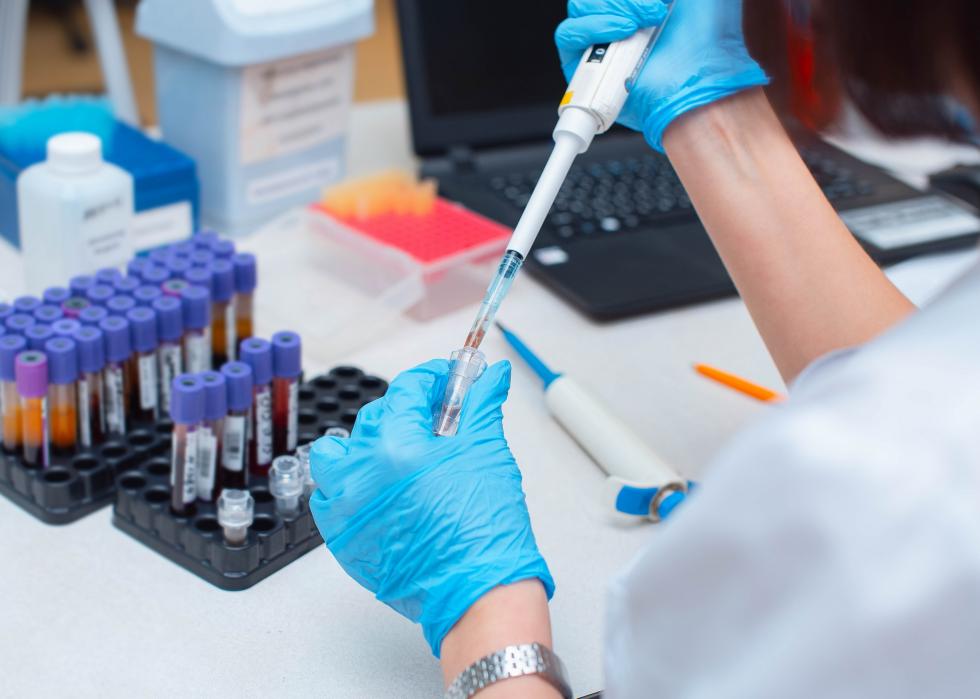
Screening for potential danger to animals
Before beginning an Investigational New Drug (IND) application, a vaccine must be screened for potential danger to animals. These take place through animal pharmacology and toxicology studies, taking preclinical data to allow an assessment as to whether the product is safe enough to begin testing in humans.

Investigational New Drug application
Once the screening for potential danger to animals is completed satisfactorily, the vaccine goes through the IND. The IND allows the vaccine sponsor to obtain permission from the FDA to distribute the vaccine across state lines to clinical investigators. At this point, the molecule being used in pharmacological activity changes legally into a new drug.
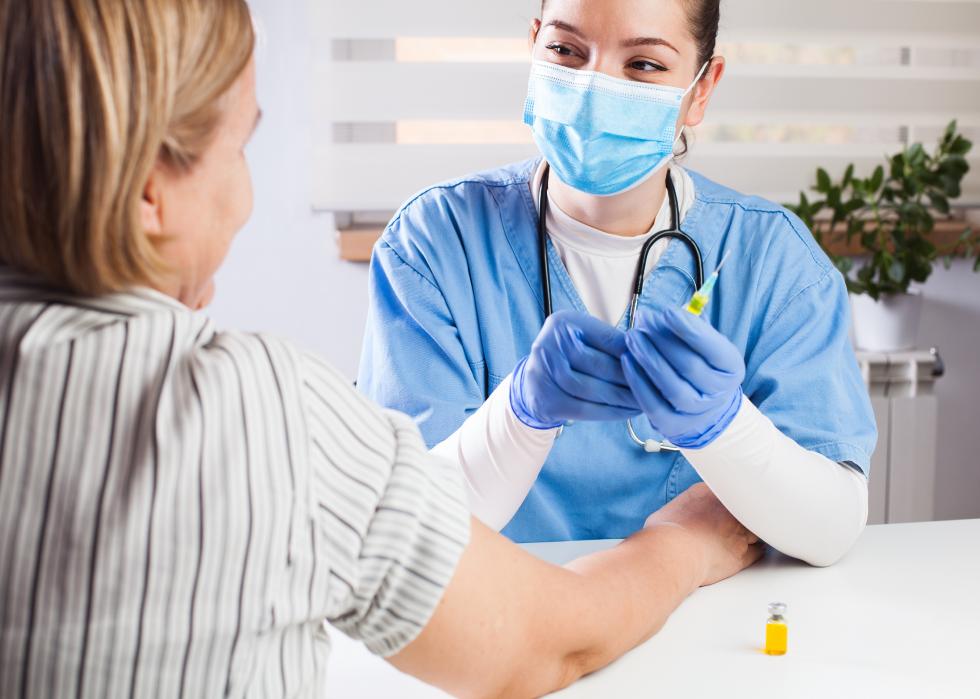
Recruiting clinical trial participants
Once a new drug is deemed safe for humans, it must be tested on humans in order to prove its efficacy and solidify its safety. A number of potential COVID-19 vaccines are already being tested on humans. However, recruiting participants is not always easy. This has been shown in the case of COVID-19 trials having difficulty recruiting Black trial participants. This is perhaps unsurprising, as Black communities have experienced medical misconduct in the past, such as the Tuskegee experiments.

Control vs. experimental groups
When enough human participants are found, the new potential vaccine is put through a randomized clinical trial, where people in the group are assigned to either a control or experimental group. The experimental group gets the vaccine, while the control group gets a placebo. Neither the people themselves nor the researchers know which group the participants are in. This does away with bias, and it is only at the end of the study that the researchers and participants find out who was in which group.
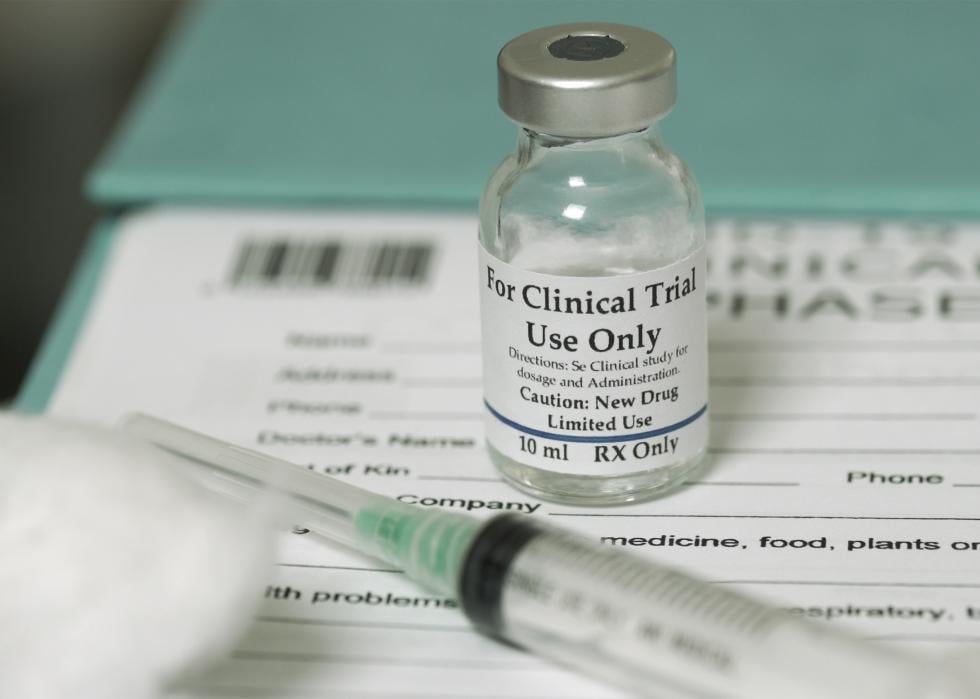
Phase 1 clinical trial
During phase 1 of the clinical trial, the first participants receive the vaccine being tested. The objectives of this phase are to evaluate the vaccine’s safety and its ability to produce the desired immune responses. It is often during this phase that the mode of giving the vaccine and the immunization schedule (how often to give the vaccine) are also assessed.

Peer review of trial results
Once a trial has results, these results must be peer reviewed. This means that expert scientists go over the data to make sure it is correct and reproducible. There have already been multiple COVID-19 vaccine candidates where phase 1 and 2 trials stood up to peer review.
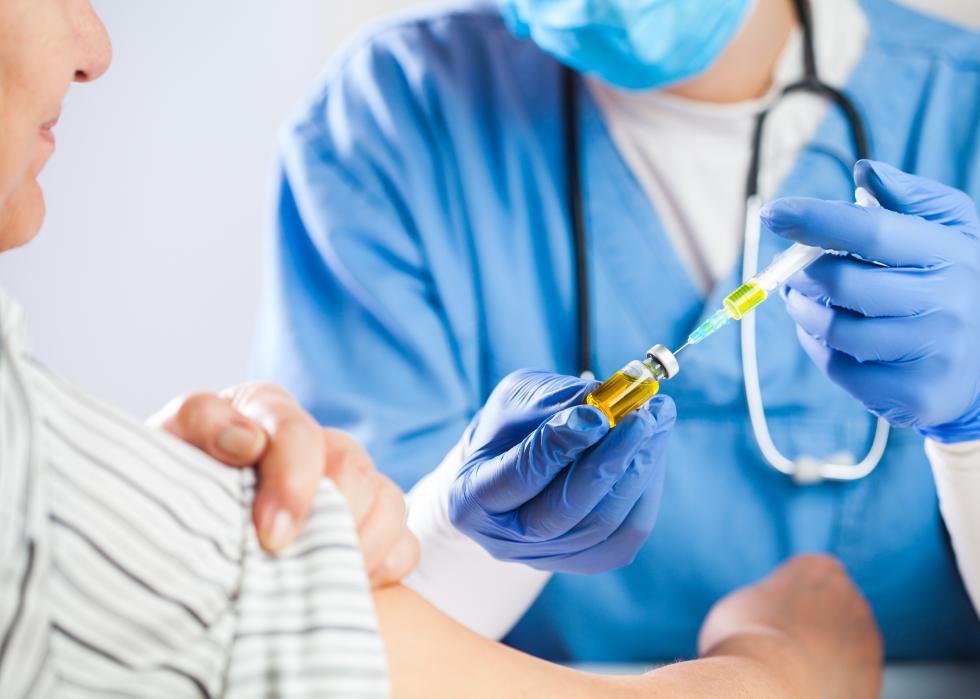
Phase 2 clinical trial
Once a candidate achieves satisfactory safety and immune response outcomes in phase 1, it moves onto the phase 2 clinical trial. Phase 2 leaves the controlled clinical setting and moves into field evaluation. This requires a steeper financial investment and therefore stricter stop-and-go policies are observed by the drug developers.
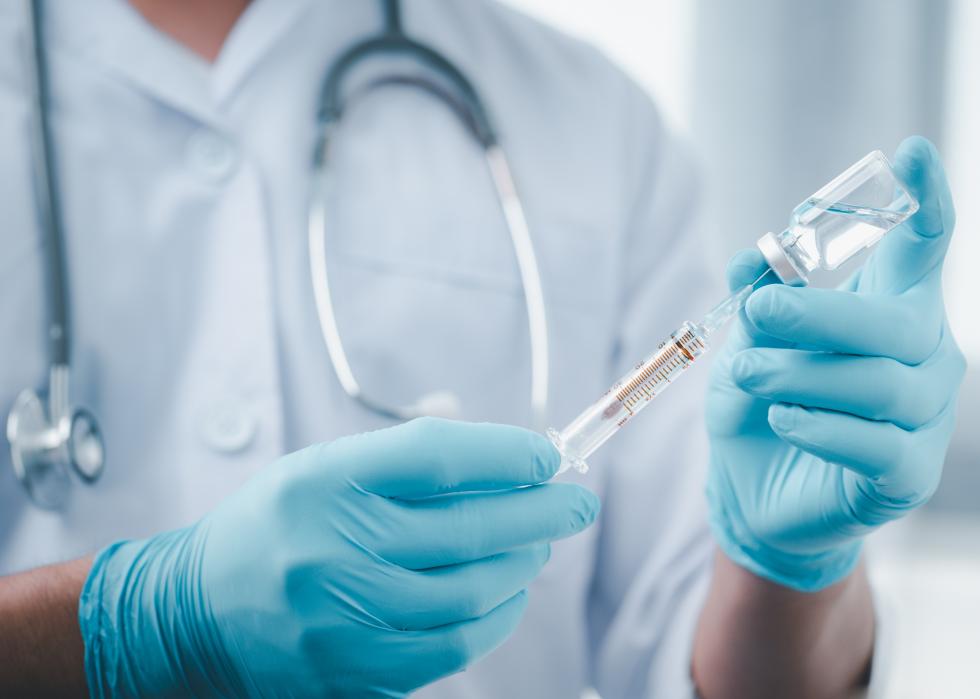
Phase 3 clinical trial
After the drug performs successfully in phase 2, it moves into the pivotal phase 3 trials, which are essential for the registration and market approval of a vaccine. These are designed to evaluate efficacy and safety. These large-scale clinical trials enroll thousands of subjects and are conducted in conditions that will be similar to the future routine use of the vaccine.

Clinical trial pause
While a lot of attention has been given to pauses in COVID-19 vaccine clinical trials, these pauses are in fact signs that the system is working and science is progressing as it should, not that vaccines are dangerous. Because vaccines are given to otherwise completely healthy people, there is a high bar for trials testing vaccines to make sure they are completely safe. Therefore, if a test participant becomes ill for any reason during a trial, the trial is paused to examine the cause of the illness.

Interim analysis
An interim analysis is done as the trial progresses in order to evaluate the effectiveness of the vaccine. In order to do an interim analysis, there need to have been enough cases of the illness among the participants to analyze the percentage that took place in the control groups as compared with the vaccinated group. The most recent COVID-19 vaccine candidate from Moderna showed a 94% success rate in its interim analysis, with only five of 95 cases of COVID-19 occurring in the vaccinated group.

Clinical trial stop
Because clinical trials are vital to progress in medicine, it is imperative that they are conducted safely. Therefore, when any ethical or safety issues are raised in the testing of a vaccine, the clinical trial is often stopped. According to the article Bioethics in Practice: Considerations for Stopping a Clinical Trial Early, “The early-stopping rule has the potential to minimize harm and to maximize benefit for the patients enrolled in a randomized trial.”

Biologics License Application
A Biologics License Application (BLA) is required to gain permission to enter a biologic product into interstate commerce. This application requires information from the applicant, who can be any legal person or entity engaged in manufacturing, along with information about the product, preclinical study information, and labeling.

Vaccines and Related Biological Products Advisory Committee
The FDA’s Vaccine and Related Biological Products Advisory Committee (VRBPAC) sets the regulatory pathway to permit wide-scale use of a vaccine and can slow down the process when it feels necessary. At the end of October, the VRBPAC held a nine-hour virtual meeting to discuss the regulatory pathway, at the end of which it told the FDA to slow down the process of trying to get a COVID-19 vaccine out so rapidly.

Manufacturing investigation
Before a vaccine can be used in the United States, the FDA must conduct a manufacturing investigation, where scientists and medical professionals investigate how the vaccine is manufactured in order to make sure it can be made consistently in a safe, pure, and potent manner. This includes inspecting manufacturing sites to ensure that they comply with regulations.

FDA approval
It is after all the aforementioned steps are carried out that a vaccine can gain FDA approval. This process can easily take a year, but in the case of COVID-19, the normally slow routine has changed. The FDA Emergency Use Authorization is allowing vaccinations to become available more quickly.

FDA Emergency Use Authorization
Emergency Use Authorization (EUA) allows the FDA to make unapproved products, such as drug treatments or vaccines, available for use during public health emergencies. However, an EUA has never been used to administer a vaccine to civilians. This is because while drug treatments are generally given to people who are already ill, vaccines are given to people who are still healthy, so the bar for using them is much higher. In the case of COVID-19, the FDA is deploying a vaccine initially under the EUA.

Vaccine supply chain
While the vaccines themselves are vital, they are only useful when they can get to the people who need them. That is where the vaccine supply chain comes in. Getting vaccines to millions of people requires effective vaccine handling, storage, and stock management, as well as rigorous temperature control and well-kept information systems.

Vaccine distribution
In the case of COVID-19, the severity of the virus makes it especially important to get the vaccine out to as many people as quickly as possible. In the United States, states are already developing vaccine distribution plans, which deal with questions of vaccine storage, data tracking, and looking at who will pay for the vaccine to be deployed and how to make sure it is done in an equitable way.

Vaccine marketing
Along with the challenges of making and distributing a vaccine, it can also be a challenge to convince people that the vaccine is safe and effective so that they will agree to get it. Before COVID-19, there was already a strong anti-vaccine movement in the United States, and science skepticism and misinformation are causing people to be wary of forthcoming COVID-19 vaccines.
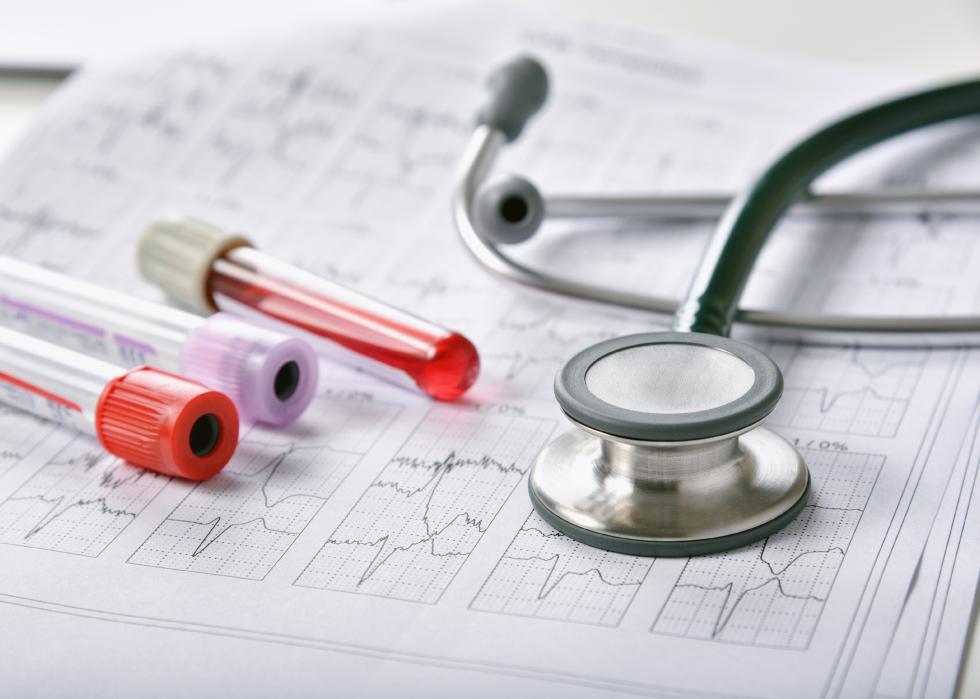
Post-marketing surveillance
Also known as a phase 4 trial, post-marketing surveillance is done once the drug is already marketed and available to the general public. This phase checks the vaccine’s performance in real life scenarios, studies the long-term risks and benefits, and potentially uncovers rare side effects.
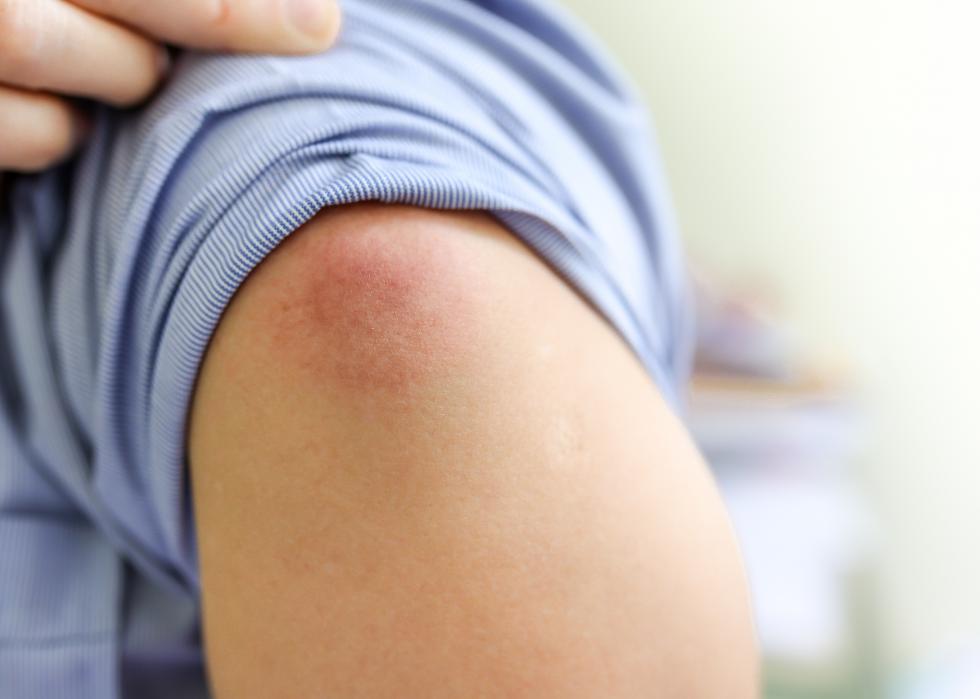
Adverse events
In the event of an adverse reaction to a vaccine, the CDC and FDA co-manage the Vaccine Adverse Event Reporting System (VAERS). This national early warning system accepts and analyzes reports of possible negative side effects after a person has received a vaccine. Anyone can report to VAERS.

Herd immunity
Herd immunity happens when a virus stops spreading because it continuously encounters people who are protected against infection. This is the ultimate aim of wide-scale vaccination programs. In this case, the vaccine protects those who are vaccinated, and herd immunity protects those who are unable to be vaccinated, for example those with compromised immune systems. The unvaccinated people become less vulnerable, because the odds that they will come into contact with an infected person decrease dramatically.



